Scar formation is a natural part of the body’s healing process after injury, surgery, burns, or chronic wounds. While scars play an important protective role by restoring the structural integrity of damaged tissue, excessive scarring or abnormal tissue remodeling can sometimes lead to functional and cosmetic concerns. In recent years, advances in regenerative medicine including research into stem cells and biologically active factors have opened new possibilities for supporting healthier tissue remodeling and improving scar outcomes.
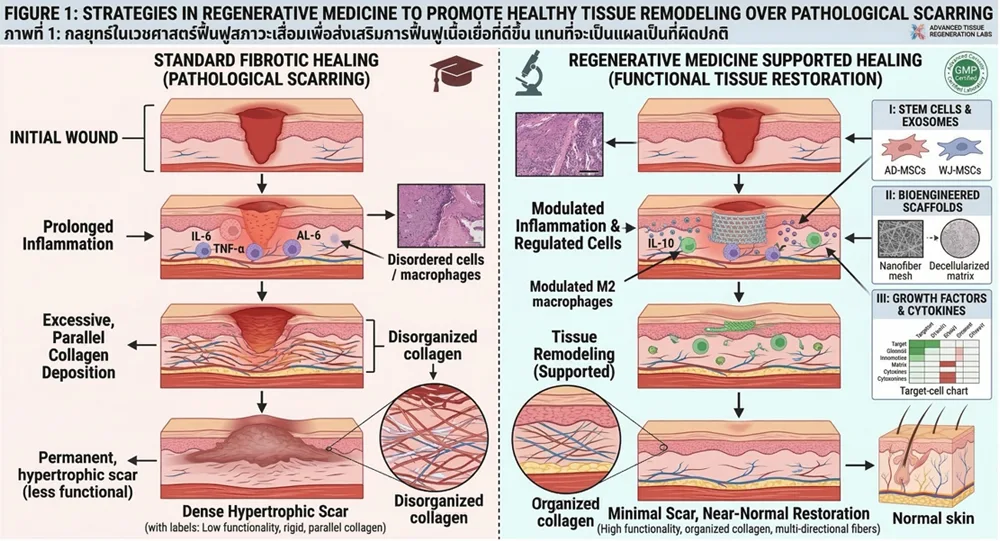
Figure 1: Comparative pathways of wound healing: Standard fibrotic scarring versus regenerative medicine-supported tissue restoration.
Understanding Scar Formation
- Hemostasis – Immediate clot formation stops bleeding and creates a temporary protective barrier.
- Inflammation – Immune cells migrate to the wound site to remove debris, bacteria, and damaged tissue.
- Proliferation – Fibroblasts produce collagen and extracellular matrix (ECM) components to rebuild tissue.
- Remodeling – Collagen fibers reorganize and mature to strengthen the repaired area.
- Hypertrophic scars – Raised scars that remain within the boundary of the original wound
- Keloid scars – Overgrown scar tissue extending beyond the wound margins
- Atrophic scars – Depressed scars commonly associated with acne or tissue loss
- Contracture scars – Tight scars that may restrict movement, particularly after burns
The Biology of Tissue Remodeling
- Collagen Reorganization Fibroblasts initially produce large amounts of type III collagen, which is rapidly deposited in the wound. Over time, this collagen is gradually replaced by type I collagen, a stronger structural protein that improves tensile strength.
- Matrix Metalloproteinases (MMPs) MMPs are enzymes that break down excess extracellular matrix. Their activity helps remove excess collagen and allows tissue to remodel into a more organized structure.
- Myofibroblast Activity Myofibroblasts are specialized cells that help close wounds by contracting the surrounding tissue. Once healing is complete, these cells normally undergo programmed cell death. If they persist, they may contribute to excessive scarring.
- Vascular Remodeling New blood vessels formed during early healing gradually regress or stabilize as tissue matures. Proper vascular remodeling ensures adequate oxygen and nutrient delivery during repair.
Factors That Influence Scar Quality
- Inflammation Prolonged inflammation is strongly associated with excessive scar formation. Elevated inflammatory cytokines may stimulate fibroblast activity and collagen deposition.
- Oxygen Supply Poor oxygenation can impair tissue repair and increase the likelihood of abnormal scar formation.
- Mechanical Stress Repeated tension on healing wounds—especially around joints—can stimulate excessive collagen production.
- Infection Wound infections prolong the inflammatory phase and disrupt normal healing pathways.
- Age and Genetics Genetic predisposition plays a significant role in the risk of hypertrophic or keloid scarring.
Emerging Regenerative Approaches in Scar Remodeling
Regenerative medicine focuses on supporting the body’s natural healing mechanisms. In recent years, researchers have investigated how biologically active therapies may influence tissue repair and scar formation.
These approaches aim to modulate inflammation, enhance cellular communication, and support healthy extracellular matrix remodeling.
Growth Factors and Paracrine Signaling
- VEGF (vascular endothelial growth factor)
- PDGF (platelet-derived growth factor)
- TGF-β (transforming growth factor beta)
- FGF (fibroblast growth factor)
Mesenchymal Stem Cells (MSCs)
Mesenchymal stem cells have received increasing attention in regenerative medicine research due to their ability to interact with the wound microenvironment.
Rather than directly replacing damaged tissue, MSCs primarily act through paracrine signaling, releasing bioactive factors that may:
- Modulate inflammatory responses
- Support angiogenesis (new blood vessel formation)
- Encourage fibroblast regulation
- Promote extracellular matrix remodeling
These mechanisms may help create conditions that favor more organized tissue repair.
Growth Factors and Paracrine Signaling
Another area of interest is the role of extracellular vesicles—tiny particles released by cells that contain proteins, RNA, and signaling molecules.
These vesicles may facilitate communication between cells during wound healing and may contribute to tissue remodeling processes.
While research continues to evolve, these biologically active components represent an exciting area of regenerative science.
Scar Remodeling and Functional Recovery
Beyond cosmetic appearance, scar tissue can also affect functional outcomes. Excessive fibrosis may restrict tissue flexibility, impair mobility, or interfere with normal organ function.
For example:
- Burn scars may limit joint movement
- Surgical scars may affect tissue elasticity
- Fibrotic scars may alter nerve or muscle function
Strategies that support balanced tissue remodeling may therefore contribute not only to improved appearance but also to better functional recovery.
Current Clinical Approaches to Scar Management
- Silicone Therapy Silicone gels and sheets are widely used to help flatten and soften scars by improving hydration and reducing collagen overproduction.
- Laser Therapy Laser-based treatments may stimulate collagen remodeling and improve scar texture.
- Microneedling Microneedling creates controlled micro-injuries that trigger collagen remodeling and may improve atrophic scars.
- Corticosteroid Injections Steroid injections may reduce inflammation and collagen production in hypertrophic or keloid scars.
Future Directions in Scar Remodeling Research
The field of regenerative medicine continues to expand, and ongoing research aims to better understand how cellular therapies and biologically active factors influence tissue repair.
Areas of active investigation include:
- Regulation of fibroblast behavior during wound healing
- Controlled modulation of inflammatory pathways
- Enhancement of extracellular matrix organization
- Optimization of angiogenesis and vascular stability
Researchers are also exploring how personalized treatment strategies may help tailor scar management based on individual biological responses.
Conclusion
Scar formation is an essential part of wound healing, but excessive or abnormal tissue remodeling can lead to functional and cosmetic concerns. Advances in regenerative medicine are helping scientists better understand the biological mechanisms that influence scar development and tissue repair.
By supporting balanced inflammation, cellular communication, and extracellular matrix remodeling, emerging regenerative approaches may contribute to healthier healing outcomes in the future.
While further clinical research is needed, the growing understanding of scar biology offers promising insights into how modern regenerative science may help improve tissue repair and recovery.
