Beyond the visible skin injury, diabetic wounds represent a deeper biological challenge that can threaten mobility, independence, and overall quality of life. In many patients, diabetic wound complications develop because prolonged high blood sugar damages blood vessels, impairs circulation, weakens immune defenses, and reduces nerve sensation in the feet and lower limbs. This combination means that even a small cut or pressure point can progress into a chronic wound that is slow to heal and vulnerable to infection. Beyond the physical burden, these wounds often carry a major psychological toll, causing stress, fear, and reduced confidence in daily life. While traditional care has focused mainly on dressing changes and basic infection control, modern diabetic wound care in Thailand is moving toward comprehensive biological and clinical support. By combining advanced wound assessment, vascular evaluation, pressure offloading, infection management, and precision wound technologies, clinicians are now able to restore the healing environment more effectively and support long-term recovery through modern diabetic wound care in Thailand.
1. The Clinical Reality of Diabetic Wounds
Diabetic wounds are often misunderstood as minor skin injuries that simply need time to close. In reality, they are a serious medical condition that can progress rapidly if not addressed early. In many diabetic patients, poor circulation reduces oxygen and nutrient delivery to the tissues, while peripheral neuropathy decreases the ability to feel pain, heat, or pressure. As a result, wounds may worsen unnoticed until infection, tissue breakdown, or deeper structural damage has already developed. This is why diabetic wound care in Thailand increasingly emphasizes early detection, routine foot surveillance, and timely intervention.
Beyond the wound itself, the emotional burden can be substantial. Patients may experience anxiety about infection, reduced mobility, prolonged recovery, or even the possibility of amputation. For years, treatment was often reactive rather than preventive. Today, however, diabetic wound care in Thailand is shifting toward a more proactive and multidisciplinary model that aims not only to close wounds, but also to preserve limb function, reduce recurrence, and support overall well-being.
2. Why Specialized Diabetic Wound Care is Necessary
The progression of a diabetic wound is not simply a matter of damaged skin. It reflects an impaired healing environment shaped by poor blood flow, repeated pressure, bacterial burden, inflammation, and metabolic imbalance. In many cases, healing is delayed because the body cannot effectively deliver oxygen, immune cells, and repair signals to the wound bed. This is why diabetic wound care in Thailand requires more than routine cleaning or standard dressings.
Specialized care focuses on identifying and correcting the factors that prevent healing. This may include pressure offloading, blood sugar optimization, vascular assessment, infection control, debridement of non-viable tissue, and the use of advanced dressings designed to maintain the right moisture balance. Through this structured approach, diabetic wound care in Thailand helps protect the tissue, reduce complications, and rebuild the conditions needed for more complete healing.
3. The Limits of Conventional Wound Protocols
- Basic Dressing Changes: Standard gauze or non-specialized dressings may cover the wound but often do not provide the ideal healing environment.
- Antibiotic-Only Strategies: Infection control is important, but antibiotics alone cannot correct poor circulation, pressure damage, or dead tissue.
- Delayed Referral: Waiting too long before involving wound specialists can allow deeper infection or tissue loss to progress.
- Limited Prevention: Treating the wound without addressing footwear, pressure points, glucose control, and vascular health increases the risk of recurrence.
4. The Therapeutic Advantage of Modern Diabetic Wound Care
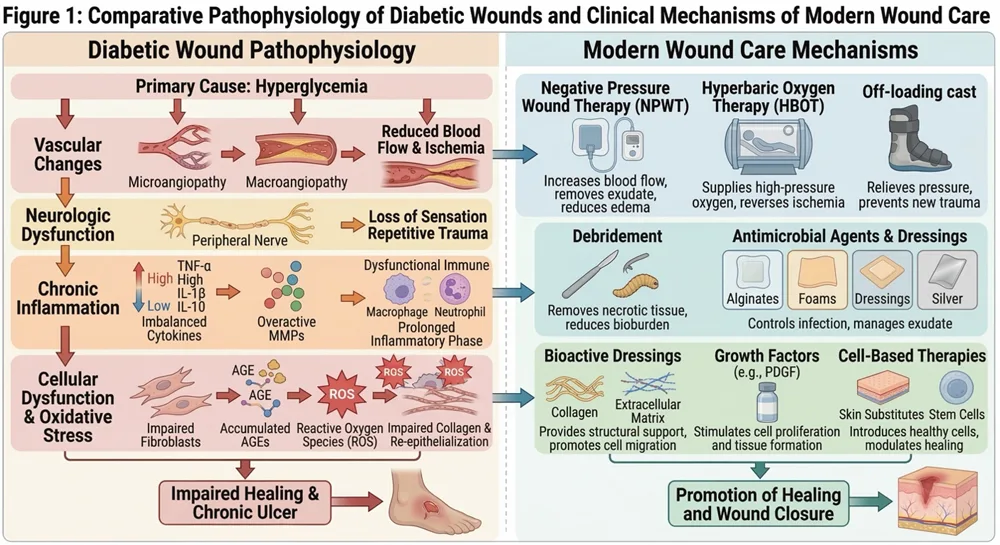
- Debridement and Wound Bed Preparation: Removing dead or infected tissue helps reduce bacterial burden and allows healthier tissue to recover.
- Moisture-Balanced Advanced Dressings: Modern wound materials are selected based on the wound’s condition to help manage fluid, protect the area, and support tissue repair.
- Pressure Offloading: Specialized footwear, padding, or offloading devices reduce repetitive stress on vulnerable areas, especially the soles of the feet.
- Vascular and Infection Management: Assessing circulation and controlling local or deep infection are essential parts of diabetic wound care in Thailand.
- Multidisciplinary Monitoring: Coordinated care involving clinicians, wound specialists, and diabetes management teams helps improve healing outcomes and reduce complications.
5. Clinical Excellence in Diabetic Wound Care in Thailand
Thailand is increasingly recognized for its growing capabilities in diabetic wound care through the integration of modern wound management, clinical expertise, and patient-centered treatment planning. This progress is supported by improved wound assessment systems, advanced dressings, infection surveillance, vascular evaluation, and a stronger emphasis on multidisciplinary care. In leading settings, diabetic wound care in Thailand involves not only local wound treatment but also a broader review of circulation, glucose control, gait mechanics, pressure distribution, and long-term prevention.
To improve outcomes, Thai specialists are placing greater attention on individualized care pathways. Rather than applying a one-size-fits-all method, diabetic wound care in Thailand is evolving toward precision-based wound management, where treatment is selected according to wound depth, infection status, tissue quality, circulation, and patient risk factors. This shift helps improve healing potential while also reducing avoidable complications, hospital admissions, and recurrence.
